The core of any Insurance plan, as we all know, is protection. Offering protection and alleviating your risk is the simple motive of an insurance plan. Making that small investment in any health insurance plan, will enable you and your clients to be tension-free and offer security in advance. Especially when we are facing the pandemic and the rising cost of treatment makes it all the more necessary to buy a Health Insurance Plan. We have all had the conversation about health insurance with our clients at least once during the last few months. As per IRDA regulation, currently, all the treatment cost incurred for Covid 19 are covered under all health insurance policies.
Though we are currently focused on the pandemic that we are faced with, as we all know, health insurance is a critical part of any person’s financial emergency toolkit and we advisors are one of the biggest advocates for that. As important as suggesting a health insurance policy is understanding the features and benefits that such a policy can cover, so that you recommend to your client what is best for them. The features breakup has been explained in 2 parts – One lesser known and the other which are generally covered.
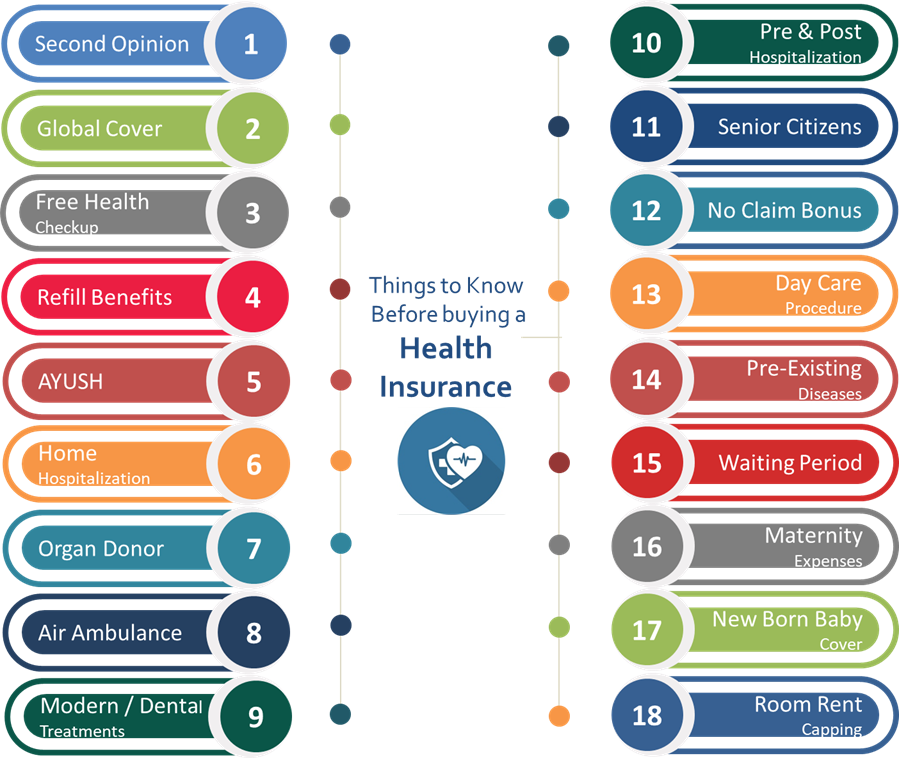
First, we go through the lesser known features –
- Second Opinion – Many insurers allow this facility for free and as an inbuilt feature from their network of medical practitioners mainly when the insured is diagnosed with a specified Critical Illness.
- Global Cover –It covers for Medical Expenses of the Insured Person incurred outside India, upto the sum insured, provided that the diagnosis was made in India and the insured travels abroad for treatment. The Medical Expenses payable shall be limited to In-patient and day-care Hospitalization only on reimbursement basis. Cashless facility may be arranged on case to case basis. The payment of any claim under this benefit will be in Indian Rupees. Insurer requires the following additional documents supporting the claim under this benefit:
a) Proof of diagnosis in India
b) Insured’s Passport and Visa
- Free Health Check-up / Preventive Health Check-Ups– Each insurer has this feature of providing Annual health checkup or once in each block of some claim-free years. The eligibility of amount and the list of tests depends as per the sum insured opted for. One can avail the same as cashless by scheduling an appointment or visit a center of your choice and claim as reimbursement.
- Restoration/Refill Benefits-When opted Sum Insured is insufficient due to claim, restoration benefit can be utilised. Multiple Restoration is available in a Policy Year for related or unrelated illnesses in addition to the Sum Insured opted for, depending upon the insurer.
- AYUSH –AYUSH treatment refers to the medical and /or hospitalisation treatments given under Ayurveda, Yoga and Naturopathy, Unani, Siddha and Homeopathy Systems. These treatments are covered only when taken at the government Hospital or in any institute recognised by government and/or accredited by Quality Council of India/ National Accreditation Board on Health. Facilities and services availed for pleasure or rejuvenation or as preventive aid, like beauty treatments, Panchakarma, purification,detoxification and rejuvenation etc are part of the exclusions.
- Home Hospitalisation or Domiciliary Hospitalisation: Domiciliary Hospitalization means medical treatment for an illness/ disease/injury which in the normal course would require care and treatment at a hospital but is actually taken while confined at home under any of the following circumstances:
- The state of the patient is such that he/she is not in a condition to be moved to a hospital for treatment, or
- The patient had to take the treatment at home in the circumstances of non-availability of a room in a hospital.
- Organ Donor- Cover for Medical and surgical Expenses of the organ donor for harvesting the organ where an Insured Person is the recipient provided that:
- The organ donor is any individual whose organ has been made available in compliance with the rules & requirements of The Transplantation of Human Organs (Amendment) Bill, 2011 and the organ which is being donated by donor is for use by the Insured Person, and
- Insurer has accepted an inpatient Hospitalization claim for the insured member under In Patient Hospitalization Treatment
- Air Ambulance–The air ambulance can be helpful in case of medical emergencies. It helps when one is injured during a trip and requires transport facility, in case one requires hospitalisation immediately and it is not possible to travel by road, etc.
- Modern Treatments and Dental Treatments – Many insurers have set defined ailments as modern Treatments like – Oral chemotherapy, robotics surgery, bariatric surgeries, stem cell therapy etc and the list is defined separately with the defined sum insured for each treatment. Dental treatment until recently was always covered in case of accident only and now after specified waiting period dental treatments like root canal, cleaning and polishing etc could be covered with defined upper limit too.
Health insurance policy would generally cover the expenditures incurred reasonably and necessarily under the following heads –
- Pre & Post Hospitalization – Medical expenditures incurred before & after the hospitalization provided that: Such Medical Costs were incurred for the same illness or the injury for which earlier and subsequent Hospitalisation was needed. And the number of days differs from insurer to insurer i.e. for pre-hospitalisation days vary from 30 days to 90 days & 60 to 180 days for post hospitalisation requirements.
- Senior Citizen Plans- There are special plans specifically designed for senior citizens and while buying them, the following points are to be considered – waiting period for pre-existing disease, Co-payment, entry age, pre-policy medicals etc.
- No Claim Bonus- In the event of no claim in the policy year, insurer adds a fixed percentage depending upon the product say from 10% rise each claim-free year subject to maximum 100% of the sum insured. Some insurers offer cumulative bonus not in excess of 200% of the sum insured under the current policy.
- Day Care Procedures –Generally an insurer covers listed Day Care Treatment due to disease/illness/Injury during the policy period taken at a hospital or a Day Care Centre. The list of treatment varies from insurer to insurer. The scope of the policy cover does not include the treatment normally taken on an out-patient basis.
- Pre – Existing Diseases- Pre-Existing Disease means any condition, ailment or injury or related condition(s) for which there were signs or symptoms, and / or were diagnosed, and / or for which medical advice / treatment was received within specified months prior to the first policy issued by the insurer and renewed continuously thereafter.
- Waiting Period- Any benefits related to pre-existing condition, ailment or injury until the defined waiting period since inception of policy, provided the pre-existing condition is disclosed in the proposal form. Claim would also not be paid for specified diseases like Cataract, stones in the urinary and biliary systems, all types of sinuses, joint replacement surgery, bariatric surgery etc. until 24 to 36 months of waiting period depending upon the insurer.
- Maternity Expenses – Most of the insurers do cover maternity benefits with specified waiting period ranging from 9 months to 72 months, the maternity cover depends upon the sum insured and covers normal delivery, C section, lawful termination of pregnancy and infertility treatment too.
- Newborn Baby Cover – It would cover Medical Expenses incurred towards treatment as inpatient for delivery. Coverage is considered under the maternity cover upto 90 days after birth and within limit of sum insured without paying any additional premium. Mandatory Vaccinations of the newborn baby up to 90 days, as recommended by the Indian Pediatric Association will be covered under the Maternity Expenses. Many insurers offer Reasonable and Customary charges for vaccination expenses for the Newborn Baby as per National Immunization Scheme (India) listed below, till the baby completes 1 year (12 months) upto the limits specified in the Schedule.
- Room Rent Capping –
- Every insurer has a thumb rule for the room rent to be charged for an admissible claim. Room rent is a sublimit set by insurers mainly under basic sum insured of a private insurer and mostly all the public sector insurers. It is generally capped at 1% of sum insured for a normal claim and 2% of the sum insured for the ICU claim. The overall billing of the hospitalisation expenses happens on the basis of the Room category opted for at the time of claim. All the other charges like nursing, medication, doctor charges, Anaesthetic doctor visit, any other expenses towards hospitalisation forms part of the room rent package selected. So while applying for claim one has to keep this fact in mind.
- However, select insurers have started to offer products where there is no room rent capping for certain levels of sum assured, thereby allowing the policy holder to be able to claim the entire room rent amount, even if it crosses the 1-2% of sum assured limits. This can be very useful, owing to the rising costs of medical treatment.
Now that you are armed with the details of these features, you can review your clients’ medical insurance recommendations and see if any updation/upgrades/changes are required therein. Please be mindful of the overall benefits from the policy and suitability to your client before making any changes for specific features. Stay informed, stay safe!
Have you come across any other such features that one must look out for? Do share with us in the comments below!
Authored by Ms. Nisha Sanghavi, Founder Fynomics
and Co-founder Promore Fintech Private Limited.

